Getting a Feel for Better Infection Control
November / December 2011
![]()
Getting a Feel for Better Infection Control
Advanced simulator for nurses addresses hospital-acquired infections.
For every 100 patients admitted to U.S. hospitals in 2002, 4.5 patients developed a nosocomial infection, also known as a hospital-acquired infection (HAI) (Graves & McGowan, 2008), and many experts believe the percentage has risen in recent years. Under new Centers for Medicare and Medicaid Services (CMS) guidelines, healthcare providers may risk partial or full denial of reimbursement for procedures where staff medical errors such as infections arise from a lack of training. With an IV catheter infection estimated to cost $100,000 in hospital care, clinical directors understand the need to improve nurse training and proficiency as an HAI risk-management activity and as a critical element of quality care and meeting patient safety goals.
As a result, healthcare organizations are exploring new options for training as part of their efforts to address the problem of infection control. One of the new options for training nurses includes advanced computer-based simulation—an approach previously used mainly in training surgical residents on specialized procedures or devices.
Practice Vs. Reality with “Dummies”
The market for medical simulation is estimated to reach $1.5 billion by 2012 (Quinn, 2010), with the dominant share of the market currently comprised of mannequin-based training for nurses and medics, along with specialized training developers. Training with mannequins at simulation centers has become a routine and valuable part of healthcare provider efforts to address patient safety both for training nurses new to a specific procedure as well as providing continuing education for experienced nurses. This is particularly true as so-called “dummies” have become increasingly high-tech with electronic displays, sensors, and readouts.
Yet mannequins have limits in their ability to address the full instructional experience of procedures. They cannot provide a learning experience that includes what a procedure “feels like” when performed on the internal organs of a patient. Achieving such experiential muscle memory is paramount to achieving proficiency in the specific procedure, as well as deeply learning every step in the process—from the first step of correctly cleansing the area to be treated, to the last step of properly applying the dressing and disposing of any waste.
“There’s a lot that’s great about mannequin-based learning, but the downside is that when a supervisor demonstrates a procedure for 5 or 6 students, then watches them each perform the procedure, the human eye can miss small steps of a procedure that are done slightly inaccurately,” said Katie Martens, APRN, CNS, a clinical learning advisor with wide-ranging hospital, long-term care and rehabilitation nursing experience. “That doesn’t begin to address the hires you don’t personally supervise.” Nor does such observation remove the variable of the instructor’s own adherence to guidelines and accurate grading. Mannequin time also requires advance scheduling, which may pose logistical constraints for the learner.
“The best training gets the student as close to the actual experience without putting the patient at risk,” Martens said.
A Clinical Reality Check
In today’s healthcare environment, time pressures due to emergencies and rushed situations caused by staffing shortages, nursing staff turnover, and patient overload make it extremely challenging to ensure quality care and can lead to deviation from safety guidelines.
Even in the best medical institutions, errors can be caused by adherence to out-of-date protocols or by experienced staffers who are experts at a procedure but may have developed bad habits over time, Martens says, and deviations from the protocol have ramifications to both quality of care and liability.
Martens relates several common deviations from IV-line infection control protocols that represent risk for the patient and liability for the hospital:
- blowing on the cleansing agents—Chlorexidine and alcohol—to speed the drying process, thereby reducing the effectiveness of the cleansing agents and breaking the sterile field;
- swabbing the cleansed area with gauze, a well-intentioned attempt to speed drying but one that itself can introduce germs;
- repeated insertion and reinsertion of a catheter, which may compromise catheter performance or increase the possibility of infection; or
- inserting the catheter into an incorrect location of the body and then re-inserting in the proper location, without changing the catheter—as with urinary catheterization in females.
Additionally, when practice guidelines change, old habits die hard—adding to the challenge of teaching the new guidelines and verifying adherence and competency. For instance, in May 2011 the Joint Commission issued a new National Patient Safety Goal for 2012 focusing on catheter-associated urinary tract infections (CAUTIs), which represents as much as 80% of HAIs in hospitals (Lo et al., 2008). It requires hospitals to ensure they follow evidenced-based practices on such steps as disposal of catheters that become contaminated due to improper insertion on the first try. Hospitals will be retraining staff to these guidelines throughout 2012.
Computer-Based Simulation: A Powerful Complement
Computer-based simulation usually places the computer in the role of anatomy instructor or procedure reviewer. The most sophisticated virtual reality simulators—those that provide immersive and lifelike sensory experiences of performing a procedure—are typically funded by medical specialty boards or device vendors and targeted toward surgical residents who will later seek accreditation from those boards or use the vendor’s devices.
These types of training experiences allow more practice opportunities during each student’s schedule than training that requires an experienced clinical supervisor, and they accommodate learners who may take longer than others without consuming undue supervisor time. While helpful, they still can lack the realism of the human, hands-on experience that mannequins can approximate. Yet few advanced simulators focus on risk and patient safety guidelines from IHI, Joint Commission, and others—and none to date target infection control.
When built using haptics (simulating the sense of touch through a machine interface), advanced 3D computer-based training simulators can combine both cognitive and kinesthetic learning, and objective evaluation. They can leverage the serious games “wow” factor to create a compelling learning experience, while achieving life-like realism—realism that has an important instructional value and ability to help decrease the incidence of infection. These types of simulators can provide kinesthetic procedural learning of the framework of the entire process, as well as the detailed specifics of the actual procedure, enabling the trainee to develop muscle memory as well as mental memory of the correct “feeling” of each step.
As such, these simulators are a powerful complement to mannequin-based training, providing unlimited practice time for the procedure, as well as the process, and highly realistic learning that can take place without the need for a supervisor. Computer-based simulators with built-in skills assessment tools can objectively evaluate each learner’s skills, pushing them to keep practicing until they’ve reached competency. These types of simulators better prepare learners to execute the procedure correctly when they train with mannequins and ultimately begin working with patients.
|
Haptics, from the Greek root haptikos, is the technology of simulating the sense of touch through a machine interface. Haptics can be either tactile or kinesthetic. Smart phones, ATMs, and game joysticks use tactile haptics, where sensors measure the pressure exerted by the user’s finger(s) and then respond by providing feedback in the form of vibration to the finger tips. In contrast, kinesthetic or force-feedback haptics allows the user to exert forces and feel the resistance that the machine delivers back—like pushing against a heavy door and feeling the sensation of your arm muscles as the weight and motion of the door resist your effort. For example, the user of a haptic device holds a stylus instead of a computer mouse, interacting with virtual objects in true 3D space and feeling the push-back when it makes contact with them. The feeling is analogous to holding a pen-sized tool and probing an object with it. Software development toolkits allow training developers to haptically-enable medical training applications, including simulating the feeling of inserting a needle through layers of skin, fluid, and muscle. |
“With advanced simulators, there’s no variability across each supervisor’s procedural understanding,” Martens said. “Everyone works to a common standard of demonstrated practice. At the end of a training, the supervisor has concrete data to say, ‘Yes, Nurse A can do this,’ or ‘Nurse B, you skipped a step.’” If someone needs a little extra time on a specific skill, they can repeat it an unlimited number of times as needed—freeing supervisor time as well.
“When simulators deliver the exact feeling of procedures, they validate for the learner what the correct procedure feels like,” Martens said. “That’s incredibly beneficial to learning.” Such advanced computer simulations can be offered if a floor or clinical department requires remediation, if its infection rate is shown to be high; when The Joint Commission issues new procedures; or for continuing education units (CEUs). They can reduce the time it takes to perform procedures and the liability posed by failing to document training and competency levels. They are allowing a new generation of clinician to be better trained and better prepared for a wider variety of cases.
Dr. Henry Pohl, vice dean for academic administration at Albany Medical College, sees an additional important educational role for 3D computer-based simulators. Dr. Pohl co-founded a local chapter of the Area Health Education Center (AHEC) to train clinicians in rural areas—clinicians who find it very difficult to get time off to travel long distances to continuing education sessions. He sees an important benefit to bringing this type of training to distant healthcare teams, allowing them to access the same valuable training experience as clinicians in high-volume urban areas.
Tactile VR for High-HAI-Risk Procedures
Because strong infection control requires both adherence to process and procedural competency, it is a fitting candidate for advanced simulation-based teaching approaches. For example, IV catheterization is a routine procedure that in practice has a failure rate of over 40% and is often associated with infection. In addition to the simple infection control steps of washing hands, wearing clean gloves, and properly cleansing the site, there is an optimal degree of force needed to pop into the vein yet not damage it—damage that can introduce possible infection and make patients uncomfortable.
One recent approach is the Tactile VR™ training solution for nurses —an intuitive, user-friendly simulator suite. Tactile VR combines eLearning with 3D haptic simulations for procedures that carry a high risk of infection based on evidence-based practice data, including peripheral IV insertion, urinary catheterization, and central venous catheterization. These are procedures where competency requires kinesthetic learning, which cannot be fully accomplished on a mannequin—and which are problematic to learn on patients.
Based on updated guidelines from IHI, The Joint Commission, and CMS, Tactile VR’s approach combines online computer-based learning with 3D haptic simulations. Learners gain core competency by first using the “Show me how” (tutorial) mode to develop a basic understanding through cognitive course components, and then by demonstrating proficiency through the computer-based simulations. The 3D graphics and haptic feedback within the simulator make the experience as realistic as possible.
The entire simulation is haptically enabled, presented in 3D, and focused on process and procedures to help prevent infection—by following each of about a dozen steps correctly. Along with learning the correct “feeling” of inserting the needle/catheter, users interact with all of the virtual objects related to the procedure in true 3D space—including feeling the clipboard as they check off each task. Graphics, sound, and force feedback provide an immersive learning experience that walks the trainee through preparatory steps of gloving and connecting the saline before it’s time to insert the catheter by “feel.”
Trainees first choose options to either “observe” and learn the procedure in a tutorial style format—or “perform,” where the simulator never corrects the learner and provides a pass/fail rating and either gives the option to receive a certificate and a CEU credit with a passing score—or, if failing, also records this. The trainee learns all steps in context.
For example, in the catheterization module, trainees choose left/right handedness, turning the cursor into a gloved hand. They then proceed to learn the procedure. A clipboard displays a checklist of each step, and the learner checks them off using the haptic device (Figure 1). The device uses technology known as proprioceptive “force feedback.” Trainees hold the device stylus just like they would hold a needle or a catheter and the device pushes back on the user’s hand when it makes contact with the virtual objects that are on screen. The training application is programmed using a software development toolkit to deliver the “real feel” of each step of the procedure—and to record training session results and competency data for trainee or supervisor review.

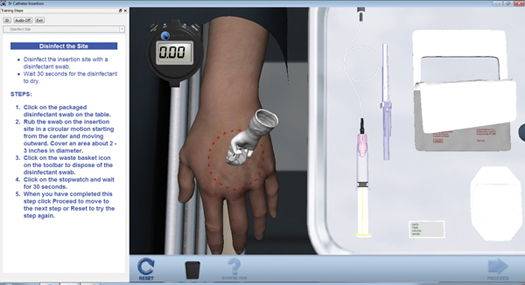
The simulation helps enforce patient safety guidelines by teaching the feel of the entire procedure. For instance, it makes trainees wait the full 30 seconds while the Chlorexidine dries, as required by the protocol—a requirement that helps the trainees experience how long 30 seconds really is (Figure 2).
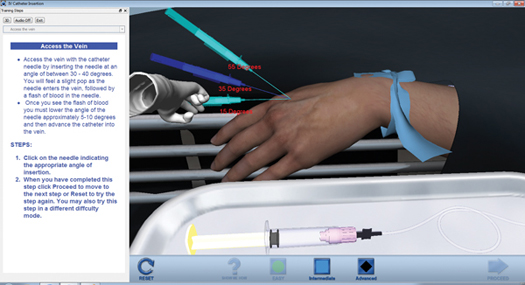
Learning the feel of properly inserting the needle/catheter is critical. In real clinical settings, the difference between the feeling of the catheter entering the vein at the correct angle of insertion is subtle but important to learn and requires practice. In Tactile VR, trainees choose from easy, intermediate, or advanced levels of difficulty, and then receive on-screen visual guidance as they feel their way through the insertion process. By incorporating haptics into the simulation, users are able to feel the difference in angles when inserting the catheter and receive visual feedback such as infiltration (skin becoming swollen) when improper angles are used (Figure 3).
When palpating to feel a vein, the trainee watches a lifelike 3D view of an arm on screen while they use the haptic device to feel for bumps that indicate a vein under the skin (Figure 4). As they insert the virtual needle, it displays in its normal color when the angle of entry is within the correct range, but turns red on screen if the trainee’s angle of entry deviates from the optimal. By learning virtually, the trainee can rotate the haptic device’s stylus from the wrist to adjust the angle up, down, around and sideways until they learn the feeling of the correct angle and force of insertion—with zero risk or discomfort to patients.

|
Tactile VR™ is a product of mySmartHealthcare, Saratoga Springs, New York. Phantom Omni® and OpenHaptics® are products of Sensable Technologies, Wilmington, Massachusetts. |
Using the haptic device, Tactile VR also quantifies the exact force exerted by the trainee and compares performance against an established Joint Commission or other standard. Trainees can review specific steps where they may need to make improvement and either receive a passing grade and a certificate or continue to practice till proficient.
Toward a More Effective Learning Approach
Additional haptically-enabled training modules using the Tactile VR platform are in development for IV therapy, tracheostomy care, and spinal tap—all procedures where developing the feeling for performing them correctly can aid in the reduction of infection. Dr. Henry Pohl of Albany Medical College participated in beta version trials at his institution, and is upbeat on the solution’s potential. “I’m very excited about Tactile VR’s unique 3D haptically-enabled approach to training nurses on IV catheterization. It offers us the opportunity to dramatically enhance our training methods and improve our evaluation of competency in this procedure—all of which will help reduce infections.”
Venkat Gourishankar is senior haptics engineer at Sensable Technologies in Wilmington, Massachusetts. He designs and engineers multisensory interfaces for human computer interaction and has extensive experience in haptic interfaces, robotics, virtual environments, and medical simulation. He has a master’s degree in mechanical engineering from the University at Buffalo and may be contacted at vgourishankar@sensable.com.
Carleigh Prodrick is marketing manager at mySmartHealthcare, Inc., in Saratoga Springs, New York. She facilitates and manages all marketing functions within the organization. She has a bachelor’s degree in communications from Le Moyne College in Syracuse, New York, and may be contacted at cprodrick@mysmarthealthcare.com.
References
Graves, N. & McGowan, J. (2008). Nosocomial infection, the deficit reduction act, and incentives for hospitals. JAMA, 300(13), 1577-1579.
Lo, E., Nicolle, L., Classen, D., Arias, A., Podgorny, K., Anderson, D. J., et al. (2008). SHEA/IDSA practice recommendation: Strategies to prevent catheter-associated urinary tract infections in acute care hospitals. Infection Control and Hospital Epidemiology, 29, S41–S50.
Quinn, K. (2010, November 24). Critical care: Surgical simulation centers advance medical learning. Training & Simulation Journal. Retrieved August 4, 2011, from http://www.tsjonline.com/story.php?F=4998557.
The Joint Commission. (2011, May 17). New 2012 national patient safety goal – Catheter-associated urinary tract infection (CAUTI). Available at http://www.jointcommission.org/new_2012_national_patient_safety_goal_cauti/.

